With its safe communities, proximity to major urban centers and beaches, and quality schools and medical centers, Connecticut is a place that many families choose to call home. But even in a state with top-rated maternity hospitals, medical errors, including those that lead to devastating conditions like hypoxic-ischemic encephalopathy (HIE), can and do happen.
If your child has recently been diagnosed with HIE, you likely have a lot of questions and concerns about their health and future, and you may be wondering if medical negligence played a role.
Don’t wait to get the answers you need. Securing your child’s future starts now.
Living with hypoxic-ischemic encephalopathy is a lifelong journey that demands substantial financial resources for comprehensive care, therapy and support. The right verdict can mean the difference between a future filled with struggle and one where your child has access to the care and therapies they need.
However, not all attorneys can navigate the complexities of birth injury cases to secure the compensation your child deserves.
Laura Brown specializes in HIE cases and understands the nuances that lead to substantial verdicts. Her expertise and dedication translate into the advocacy your family needs during this challenging time.
Due to strict legal deadlines, the window for action is limited, and every moment counts when it comes to preparing a compelling case to secure your child’s well-being for a lifetime.
Reach out to Brown Trial Firm today to schedule your consultation.
What is hypoxic ischemic encephalopathy?
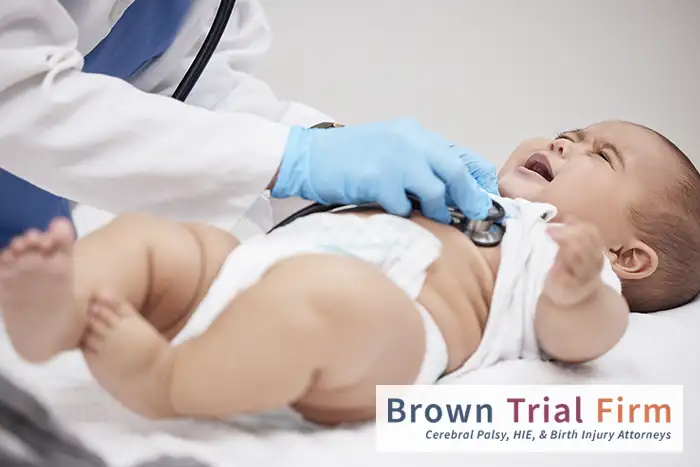
Hypoxic-ischemic encephalopathy (HIE) is a condition that occurs when the brain does not receive enough oxygen and blood. This can lead to a range of complications, including cognitive impairments, physical disabilities, and even death in severe cases.
HIE is most commonly seen in newborns, particularly those who have experienced a difficult birth, although it can also occur in older individuals under certain circumstances, such as cardiac arrest or severe trauma.
The term “hypoxic” refers to a lack of oxygen, and “ischemic” refers to a lack of blood flow. “Encephalopathy” means a disorder or disease of the brain. So, HIE involves both oxygen and blood flow deficiencies that lead to brain damage.
A guide to baby brain damage
Understand when infant brain damage might be the result of medical negligence.
The connection between preterm birth and HIE
With a preterm birth rate of 9.6% in 2022, Connecticut was given a “C+” grade on the March of Dimes “Report Card.” Surprisingly, this is a slightly better grade than the overall U.S., which received a “D+” grade in 2022 for a preterm birth rate of 10.5%.
Why does this matter?
Preterm births are associated with an increased risk of HIE compared to full-term births. Preterm infants, particularly those born before 32 weeks of gestation, have immature organ systems, including the brain and lungs, which makes them more vulnerable to complications such as insufficient oxygen and reduced blood flow. Additionally, preterm infants are more susceptible to infections, another risk factor for HIE.
Because of this, it’s crucial that pregnant mothers in Connecticut and throughout the U.S. have access to adequate prenatal care to prevent HIE and other complications in babies related to preterm births.
What are the symptoms of a baby with HIE?
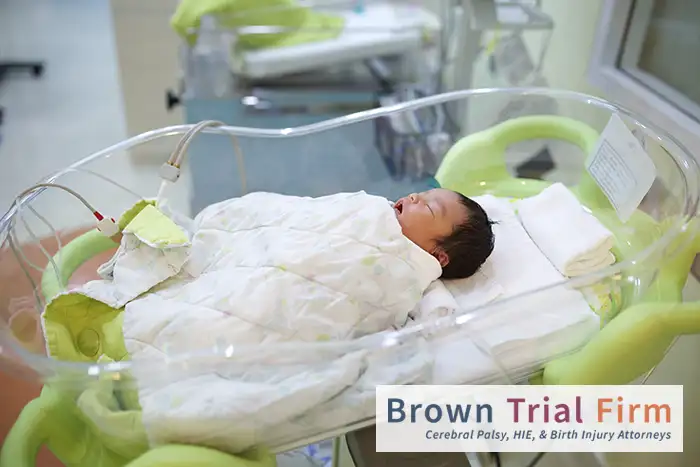
The symptoms of HIE in a newborn can vary in severity from mild to severe. In many cases, these symptoms appear immediately after birth, but in some instances, they may not be evident for months or even years.
Some common symptoms in babies include:
- Low Apgar scores, usually below 3 for the first 5 minutes after birth
- Difficulty breathing or absence of breathing immediately after birth
- Weak or absent reflexes, such as the sucking or grasping reflex
- Trouble hearing or responding to sounds
- Poor muscle tone, often described as “floppy” or “limp”
- Abnormal movements, such as seizures or spasms
- Bluish or pale skin color
- Reduced level of consciousness or responsiveness
- Feeding difficulties, including trouble latching or swallowing
- Abnormal heart rates and blood sugar levels (either too high or too low)
Babies with mild HIE may show fewer or less severe symptoms, which may resolve over time with appropriate treatment. However, severe cases can lead to long-term complications and may require intensive intervention, including resuscitative measures, medications, and potentially therapeutic hypothermia.
Prompt recognition and treatment of HIE are critical to improving outcomes and minimizing potential long-term damage. If you suspect that your newborn is experiencing symptoms of HIE, seek medical attention immediately.
Our baby was perfectly healthy throughout the pregnancy, but after a chaotic birth, we were told he has HIE. It’s hard not to question whether a medical mistake was made.
What signs might an older baby or toddler with HIE exhibit?
In some babies, HIE symptoms may not be evident immediately after birth but could become noticeable as the child grows and reaches developmental milestones. Here are some signs that an older baby or toddler with HIE might exhibit:
- Developmental delays. Slower achievement of developmental milestones like sitting, crawling, walking or talking
- Cognitive issues. Difficulties with memory, problem-solving, and learning
- Motor skill impairments. Weakness, poor coordination, and difficulties with fine and gross motor skills
- Speech delays. Slower speech development, difficulties with articulation or challenges in language comprehension
- Behavioral problems. Issues such as hyperactivity, impulsiveness or difficulties with social interaction
- Epilepsy. Ongoing seizures that may require medication for control
- Feeding difficulties. Challenges with chewing, swallowing or digesting food
- Vision or hearing impairments. Problems like poor eye coordination, partial or total vision loss, or hearing deficits
- Sensory issues. Increased or decreased sensitivity to pain, touch or other sensory stimuli
- Sleep disturbances. Irregular sleep patterns, difficulty falling asleep, or frequent waking
Connecticut HIE attorney Laura Brown is proud to be able to help families get results like these:
$10.3
Million
HIE & cerebral palsy birth injury
Mateo Ramirez was diagnosed with cerebral palsy when, as an infant, he suffered severe injuries by suffocating on his mother’s umbilical cord. After hearing the evidence we presented, the jury in Brownsville, Texas returned a verdict for $10.3 million for the child’s medical expenses over the course of his life. The Ramirez family is relieved that Mateo will be able to receive the vital medical care he needs.
Interested in learning what Laura Brown can do for your family? Contact Brown Trial Firm to schedule your free consultation.
It’s essential to note that not all children who have HIE at birth will show these symptoms. The range and severity of symptoms depend on various factors, including the extent of the brain injury, the effectiveness of initial treatment, and ongoing therapy and intervention.
Additionally, other medical conditions and birth injuries can have similar symptoms, so it’s crucial to seek a diagnosis from a health care provider to ensure your child receives the appropriate treatment.
What are the most common causes of HIE in babies?
HIE in babies can result from a variety of factors that lead to reduced oxygen and blood flow to the brain. It’s important to understand that complications that lead to HIE can occur at any time during pregnancy, labor or delivery.
Common causes include the following:
- Prolonged labor. If labor fails to progress and the baby shows signs of distress, failure to perform a necessary cesarean section (C-section) can lead to reduced oxygen and blood to the baby.
- Prolapsed umbilical cord. This occurs when the umbilical cord slips into the birth canal ahead of the baby, which can cause compression and restricted blood flow.
- Uterine rupture. This is a rare but severe complication where the uterus tears, often endangering both mother and baby.
- Meconium aspiration. Inhalation of meconium (the baby’s first feces) into the lungs can cause respiratory issues and reduced oxygen levels that can lead to HIE.
- Uterine hyperstimulation. Drugs like Pitocin can cause the uterus to contract too forcefully or too often, leading to impaired oxygen to the fetus.
- Kernicterus. Untreated or mismanaged jaundice in a newborn can lead to a condition called kernicterus, which is a type of brain damage that occurs because of a buildup of a substance called bilirubin, leading to oxygen deprivation.
- Placental abruption. This is a premature separation of the placenta from the uterine wall, which reduces the flow of nutrients and oxygen to the baby.
- Placental insufficiency. This is a condition in which the placenta fails to deliver adequate nutrients and oxygen to the fetus, leading to inadequate oxygen and nutrient delivery to the fetus.
- Asphyxia during birth. This refers to an interruption of oxygen supply during labor and delivery, often due to umbilical cord problems or prolonged labor.
- Maternal blood pressure issues. Both low and high blood pressure in the mother can lead to reduced blood flow to the placenta and, consequently, to the baby. It’s crucial that doctors monitor a pregnant woman’s blood pressure throughout pregnancy and prescribe medications to control it when medically indicated.
- Birth trauma. Physical injury during delivery, such as the use of forceps or vacuum extraction, can sometimes cause HIE if it leads to blood loss or reduced oxygen supply.
- Infection. Maternal or fetal infections can lead to inflammation, affecting both the placenta and the baby’s oxygen levels.
It’s important to note that while these are common causes, HIE can sometimes occur without a clear reason. Quick recognition and immediate medical intervention are crucial for improving outcomes in babies who have HIE.
What is the best treatment for hypoxic-ischemic encephalopathy?
The best treatment for HIE in newborns often involves a combination of immediate resuscitative measures and advanced therapies, with therapeutic hypothermia, also called brain cooling, being the most widely recognized and evidence-based treatment for moderate to severe cases.
Therapeutic hypothermia involves cooling the baby’s body to a few degrees below normal body temperature for a set period, usually 72 hours, to reduce metabolic demand and protect the brain from further damage. It’s crucial to initiate treatment as soon as possible, ideally within 6 hours after birth, to maximize its effectiveness.
Additional treatments may include respiratory support, anti-seizure medications, and close monitoring in a neonatal intensive care unit (NICU).
Birth injury attorney Laura Brown discusses brain cooling treatment for newborns
Learn about brain cooling treatment, including when and how it should be administered to infants to prevent brain damage.
What is the survival rate for hypoxic-ischemic encephalopathy?
According to some recent studies published in the National Library of Medicine and PLOS One, about 1 in 4 infants born with HIE die from the condition. Infants with mild HIE who receive prompt and appropriate treatment have a much higher survival rate, while those with severe HIE often have lower survival rates and are at a greater risk for long-term complications.
As medical treatments continue to advance, outcomes for infants with HIE may improve, but early recognition and immediate intervention remain crucial for increasing the chances of survival and reducing long-term impairments.
Can HIE be cured?
Hypoxic-ischemic encephalopathy cannot be completely cured, but early intervention and appropriate treatment can significantly improve outcomes and potentially minimize long-term complications. Even with effective treatment, some babies may still experience lasting effects of brain injury, such as developmental delays, cognitive impairments, and motor skill issues.
Ongoing therapies like physical, speech and occupational therapy can help manage these symptoms and improve quality of life. However, the severity of HIE, the timeliness of treatment, and other individual factors will influence long-term outcomes.
What is the life expectancy of a baby with HIE?
While studies have shown that about 25% of infants die from HIE, the life expectancy of those who survive will vary based on the severity of their condition as well as other health issues they may have.
In mild cases of HIE where treatment is prompt and effective, many children may go on to have a normal life expectancy. However, moderate to severe cases can result in significant neurological or developmental impairments, like epilepsy or cerebral palsy, that could affect life expectancy and quality of life.
If you’re dealing with a case of HIE, consultation with health care providers for a thorough evaluation and personalized treatment plan is crucial for understanding the potential long-term outlook.
Prognosis and life expectancy for HIE
Learn about some of the factors that affect life expectancy and quality of life in children with HIE.
How do I know if my baby’s HIE was caused by a medical mistake?
Determining if your baby’s hypoxic-ischemic encephalopathy was caused by medical negligence requires a thorough investigation, often involving medical experts, legal consultation, and a detailed review of medical records.
The term “medical negligence” refers to a failure on the part of a health care provider to meet the standard of care that is generally accepted in the medical community for a particular situation.
Mistakes that could potentially be classified as medical negligence leading to HIE might include:
- Failure to provide adequate prenatal care
- Failure to diagnose or treat medical conditions in the mother or baby
- Failure to monitor fetal distress signs before, during or after delivery
- Incorrect use of delivery instruments like forceps or vacuum extractors
- Failure to perform a timely C-section in the face of complications
If you suspect that your baby’s HIE was caused by a medical mistake, it’s crucial to consult with a medical malpractice lawyer who specializes in birth injuries. They can help guide the process of collecting evidence, securing expert opinions, and, if necessary, taking legal action to seek compensation.
Are you concerned your baby’s HIE was caused by a doctor’s mistake? Get help from experienced Connecticut HIE birth injury attorney Laura Brown.
At Brown Trial Firm, we understand how devastating a diagnosis of HIE can be for children and their families. The medical, emotional and financial toll can be overwhelming, especially if you suspect that medical negligence may have played a role. But you don’t have to navigate this challenging process alone.
Experienced Connecticut HIE attorney Laura Brown offers free consultations to assess the details of your case and help you understand your legal options.
Protect your child’s future and secure the support your family deserves by contacting Brown Trial Firm today to schedule your appointment.
Are you an attorney handling an HIE case in need of specialized birth injury expertise?
If so, look no further than Brown Trial Firm, where Laura Brown has distinguished herself as a dedicated HIE case specialist with a proven success record nationwide. Understanding the unique challenges and complexities that come with HIE litigation, Laura and her expert team offer unparalleled legal representation in this highly specialized field.
When you collaborate with Brown Trial Firm, you’re not just acquiring a co-counsel; you’re gaining a valuable ally. Benefit from expertise in HIE litigation, access to leading medical experts, and an unwavering commitment to securing the best outcomes for the families you represent. Elevate your client’s chances for a favorable verdict by partnering with Laura Brown and her exceptional team today.
References
2022 March Of Dimes Report Card For Connecticut. (n.d.). March of Dimes | PeriStats. Retrieved October 18, 2023, from https://www.marchofdimes.org/peristats/reports/connecticut/report-card
Ezenwa, B. N., Olorunfemi, G., Fajolu, I., Adeniyi, T., Oleolo-Ayodeji, K., Kene-Udemezue, B., Olamijulo, J. A., & Ezeaka, C. (2021). Trends and predictors of in-hospital mortality among babies with hypoxic ischaemic encephalopathy at a tertiary hospital in Nigeria: A retrospective cohort study. PLOS ONE, 16(4), e0250633. https://doi.org/10.1371/journal.pone.0250633
Namusoke, H., Nannyonga, M. M., Ssebunya, R., Nakibuuka, V. K., & Mworozi, E. (2018). Incidence and short term outcomes of neonates with hypoxic ischemic encephalopathy in a Peri Urban teaching hospital, Uganda: a prospective cohort study. Maternal Health, Neonatology and Perinatology, 4(1). https://doi.org/10.1186/s40748-018-0074-4