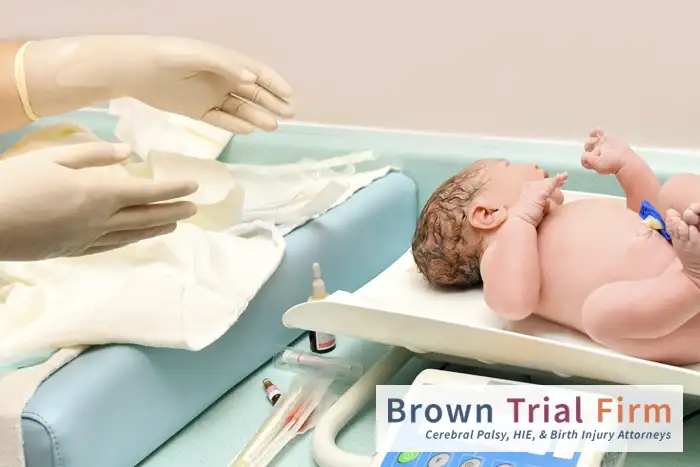
The journey of pregnancy is an awe-inspiring process in which the little life growing inside the mother’s womb undergoes remarkable development in just a few months’ time. During this crucial period, the developing brain of the unborn baby is particularly vulnerable to injury, and any harm can have lifelong consequences.
Brain damage during pregnancy or delivery may be immediately apparent, or it might not be noticeable for many months or even years later as your child begins to show signs of developmental delays.
If you’ve recently discovered your child is suffering from brain damage, you owe it to them and yourself to understand the potential causes and determine if medical negligence played a role. Consulting with an experienced birth injury attorney is an important first step to getting your child the compensation they need for medical care and treatments so they can live their life to the fullest.
Jump to section
- Common types of brain damage in newborns
- How to know if a baby has brain damage
- What are some signs of brain damage in older babies and toddlers?
- Common causes of brain damage in newborns
- How long does brain damage take to show?
- Can a baby recover from brain damage?
- Can an MRI detect brain damage in a newborn?
- Can a long labor cause brain damage?
- Is there any treatment for newborn brain damage?
- How cooling therapy impacts brain damage in infants
- What treatments are available to older children diagnosed with brain damage?
- Can a baby swing cause brain damage?
- Can babies get brain damage from hitting their heads?
- What are the signs of brain damage in babies after a fall?
- Could dropping a baby cause brain damage?
- Can leaving a baby to cry damage their brain development?
- Can throwing a baby in the air cause brain damage?
- How can the timing of a brain injury influence a baby’s development?
Common types of brain damage in newborns
Below are some of the most common forms of brain damage that occur during pregnancy, labor and delivery. If your baby has been diagnosed with any of these conditions, it’s imperative to investigate if medical negligence played a role in their brain damage:
- Cerebral palsy. Cerebral palsy is a condition characterized by impaired muscle control and movement resulting from a brain injury, usually occurring during birth or early childhood. It can lead to lifelong physical disabilities, affecting an individual’s ability to perform everyday tasks and requiring specialized care and support.
- Hypoxic-ischemic encephalopathy (HIE). HIE is a condition that results from insufficient oxygen levels during pregnancy, labor or delivery. It can happen due to various factors, including complications during labor and delivery, umbilical cord problems, placental issues, maternal blood pressure problems, or uterine rupture. HIE can result in brain damage and lead to long-term developmental delays and disabilities for the affected child.
- Spastic diplegia (spasticity in the legs). Spastic diplegia is a form of cerebral palsy characterized by increased muscle tone and stiffness, primarily affecting the legs. It results from brain damage or injury during early development, leading to motor and movement difficulties. Children with spastic diplegia often experience challenges in walking, balance, and coordination and may require specialized therapies and interventions to manage their condition and improve their quality of life.
- Neonatal intracranial hemorrhage (childbirth brain bleeds). Neonatal intracranial hemorrhage, also known as a brain bleed, refers to bleeding that occurs within the baby’s skull or around the brain shortly after birth. These brain bleeds can range in severity and may have long-term consequences for the baby’s health and development.
- Hydrocephalus (extra fluid in the brain cavity). Hydrocephalus is a condition characterized by an accumulation of cerebrospinal fluid within the brain’s cavities, leading to increased pressure and swelling. This condition can be present at birth or develop shortly afterward, and it may result in various neurological issues if left untreated.
- Hemiplegia (brain or spinal cord injury). Hemiplegia is a type of paralysis that affects one side of the body, typically caused by a brain or spinal cord injury. It results in the loss of movement and sensation on the affected side, leading to challenges in mobility and daily activities for those affected.
- Hemorrhagic stroke. Hemorrhagic strokes in newborns are rare but serious medical conditions characterized by bleeding in the brain. They can occur due to various factors, such as birth trauma or complications, blood clotting disorders and infections. These strokes can lead to significant brain damage and long-term neurological complications for the child.
- Neonatal stroke. A neonatal stroke is a type of stroke that occurs in newborn babies, typically within the first 28 days of life. It’s caused by a disruption of blood flow to the brain and can result in various neurological impairments, developmental delays, and long-term health complications.
- Periventricular leukomalacia (PVL) brain injury. PVL is a type of brain injury that primarily affects premature infants. It involves the death or damage of white matter in the brain, which can lead to neurological and developmental problems. PVL is often associated with oxygen deprivation or blood flow issues during the prenatal or perinatal period.
- Infant seizures. Infant seizures refer to abnormal and uncontrolled electrical activity in a baby’s brain, resulting in sudden movements or changes in behavior. Seizures in infants can be caused by various factors, including brain injuries during birth, infections, metabolic disorders and genetic conditions.
- Cervical dystonia. Cervical dystonia, also known as spasmodic torticollis, is a neurological disorder characterized by involuntary muscle contractions in the neck, causing the head to twist or turn in abnormal positions. This condition can lead to pain, discomfort and limited range of motion in the neck, affecting the child’s quality of life.
- Jaundice (kernicterus). Kernicterus is a condition that occurs when a newborn’s high bilirubin levels (jaundice) cause brain damage. It can result in severe neurological impairments, including developmental delays, hearing loss and movement difficulties.
- Caput succedaneum and cephalohematoma. These conditions are often the result of an improper use of forceps or a vacuum extractor. Caput succedaneum is a condition where swelling and bruising occur on the baby’s scalp due to pressure during birth that typically resolves on its own. A cephalohematoma involves bleeding beneath the baby’s cranial bone caused by trauma during birth. While it might require medical attention, it usually resolves over time.
What are the top medical errors that cause birth injuries?
Learn about these top medical mistakes that frequently lead to birth injuries.
How to know if a baby has brain damage
If a baby experiences complications from pregnancy, labor, delivery or a head injury in their first months of life, parents often worry about brain damage. In some cases, you might see physical signs of trauma, but it might also be necessary to observe a child for developmental delays associated with brain damage.
Here are a few of the early signs of baby brain damage to watch out for in your infant or toddler:
- Overly large forehead or undersized head
- Inability to move or focus their eyes properly
- Distorted facial features
- Unexplained seizures
- Stiffness in their neck
- Intense or prolonged crying with an arched back
- Limp neck or inability to lift their head
- Feeding problems
- Unusual sleeping patterns
If you see any of these signs of brain damage in your baby, it’s crucial to seek out a medical diagnosis and treatment from a qualified health care professional as soon as possible to minimize the potential long-term consequences.
If you suspect that your baby’s symptoms may be the result of a medical mistake, be sure to consult a birth injury attorney or newborn seizures lawyer to discuss the details of your child’s case and potential legal options for compensation.
What are some signs of brain damage in older babies and toddlers?
As your baby moves past 6 months of age, the symptoms of brain damage may become more obvious as they struggle to meet developmental milestones.
For instance, your baby might not be able to lift their head at 6 months or roll over on their own by the time they’re 9 months old.
Working with a pediatrician to determine if your baby is meeting the established milestone markers is crucial for identifying if they suffered baby brain damage during pregnancy, labor or shortly after birth.
Apgar scores & birth injuries
Understand when a low apgar score could be a sign of medical negligence.
Common causes of brain damage in newborns
Newborn brain damage is usually the result of oxygen deprivation, also known as perinatal asphyxia. When a baby experiences a lack of oxygen in the womb, it can cause their brain cells to become damaged or die, leading to potential neurological deficits and even death.
Immediate medical attention and interventions, such as resuscitation and oxygen administration, are vital to mitigate the effects of low oxygen levels and prevent long-term brain damage in infants.
Below are some of the most common causes of oxygen deprivation during pregnancy, labor and childbirth that often lead to brain damage:
- Fetal intolerance to labor. Fetal intolerance to labor refers to a condition where the fetus exhibits signs of distress or an inability to tolerate the stress of labor, usually due to a lack of oxygen. It often leads to medical interventions to ensure the safety and well-being of the unborn baby during childbirth.
- Placental problems. Placental problems, such as placental abruption and placenta previa, can result in insufficient blood flow, depriving the baby’s brain of vital oxygen and potentially leading to brain injuries and long-term neurological consequences.
- Umbilical cord problems. Umbilical cord issues like cord compression, prolapse or knots can compromise the baby’s vital oxygen intake, potentially causing brain injuries.
- Uterine rupture. This rare but serious complication occurs when the uterus tears open, potentially causing severe hemorrhage and depriving the baby of essential nutrients and oxygen, leading to brain injury and other life-threatening consequences.
- Cephalopelvic disproportion. Cephalopelvic disproportion occurs when the baby’s head is too large or the mother’s pelvis is too narrow for a vaginal delivery. In such cases, prolonged labor or obstructed birth can result in oxygen deprivation to the baby’s brain, leading to potential brain damage.
- Meconium aspiration syndrome. Meconium aspiration syndrome occurs when a baby inhales meconium (the first stool) into their lungs before or during birth. This is more likely to happen if the fetus is under stress during labor. The meconium can obstruct the airways and lead to breathing difficulties, which may cause a lack of oxygen to the brain, resulting in brain damage.
- Amniotic fluid embolism. Amniotic fluid embolism is a rare but serious condition that can occur during pregnancy and labor when amniotic fluid or fetal cells enter the mother’s bloodstream and cause an allergic-like reaction. The rapid release of chemicals in response to this event can lead to severe respiratory and cardiovascular complications in both mother and fetus, potentially leading to brain damage due to oxygen deprivation.
- Premature delivery. Premature delivery, also known as preterm birth, refers to the birth of a baby before 37 weeks of pregnancy. Babies born prematurely are at a higher risk of various health complications, including brain damage, due to underdeveloped organs and systems. The immature brain is particularly vulnerable, and proper medical care and interventions immediately after birth are crucial to minimize the risk of brain injury and improve the long-term outcomes for these babies.
- Infections at birth. Infections can pose serious risks to newborns and may lead to brain damage. When a baby is exposed to harmful bacteria or viruses during the labor and delivery process, there is a potential for the infection to affect the brain, leading to conditions such as meningitis or encephalitis.
- Maternal infections during pregnancy. Maternal infections during pregnancy can pose serious risks to both the mother and the developing baby. Certain infections, like cytomegalovirus (CMV), rubella, chickenpox and toxoplasmosis, can be transmitted to the fetus and cause birth defects, brain damage, seizures and even death.
- Mismanaged fetal malposition. Mismanaged fetal malposition refers to situations during labor and delivery where the baby is not in the correct position for birth. This can lead to a prolonged and difficult labor, increasing the risk of complications like oxygen deprivation and birth injuries. When healthcare providers fail to recognize and address fetal malposition in a timely and appropriate manner, it can result in preventable birth injuries and long-term health issues for the baby, like brain damage.
- Oligohydramnios (low amniotic fluid). Oligohydramnios, also known as low amniotic fluid, is a condition in which the volume of amniotic fluid surrounding the baby in the womb is lower than normal. This condition can lead to complications during pregnancy and childbirth, such as an increased risk of birth defects, preterm labor, and issues with the baby’s lung development, which can lead to brain damage.
- Improperly managed or undiagnosed gestational diabetes. Improperly managed or undiagnosed gestational diabetes (high blood sugar levels occur during pregnancy) can cause various birth complications, including stillbirth and macrosomia (a large baby), which can lead to birth injuries and brain damage.
Prolonged labor and delay in performing cesarean section lawyer
Learn when a failure to perform a C-section during a prolonged labor could be medical negligence.
How long does brain damage take to show?
The time it takes for brain damage to become evident after birth depends on many factors, including the cause and severity. Some instances of brain damage can be identified immediately after birth, while others may not be noticeable for a few months or even years.
Here are a few examples:
- Acute birth trauma. In cases of traumatic brain injury during the birthing process, such as a severe head injury or lack of oxygen, signs of brain damage may be apparent immediately or within a few hours after birth. This can manifest as seizures, abnormal reflexes, abnormal breathing patterns or other neurological symptoms.
- Hypoxic-ischemic encephalopathy. The signs of brain damage from HIE may not be immediately apparent and can emerge over the first few days or weeks of life, although it sometimes takes up to 4 years before the severity of HIE brain damage is fully evident. The signs may include lethargy, difficulty feeding, abnormal muscle tone, seizures or developmental delays.
- Infection or illness. Infections such as meningitis or encephalitis can cause brain damage in newborns. The signs and symptoms of brain damage in these cases may develop over a period of days or weeks and can include fever, irritability, poor feeding, seizures or changes in consciousness.
- Genetic or congenital conditions. Some forms of brain damage in newborns may be due to genetic or congenital conditions. The signs of brain damage in these cases can vary widely and may become apparent soon after birth or in the following months as developmental milestones are missed or delayed.
Birth injuries vs. birth defects: What’s the difference?
Learn about the main differences between a birth injury and a birth defect and how it affects your ability to pursue compensation.
Can a baby recover from brain damage?
If an infant has extremely mild brain damage, they may be able to make a full recovery. Unfortunately, this isn’t the case with most forms of brain trauma. Experiencing a prolonged lack of oxygen at birth can lead to trauma that a baby’s brain can’t recover from, and this often leads to lifelong disabilities.
Monitoring an infant for signs of brain damage immediately after birth is critical, as early treatments and therapies may help reduce the lifelong effects it has on their development.
Can an MRI detect brain damage in a newborn?
Yes, an MRI is an effective tool for determining if a baby has brain damage. They’re most effective when done early enough to allow action to be taken to prevent the worst effects of trauma. For instance, an MRI could detect a brain bleed or swelling in a newborn while there is still time to use medical intervention to reduce the chances of severe damage.
It’s important to note that some brain injuries take time to appear on an imaging scan. For this reason, your baby’s medical team might request multiple imaging tests over time to help them identify and track a developing brain injury.
Can a long labor cause brain damage?
Yes, prolonged labor without medical intervention is a common cause of brain damage in babies. When labor is prolonged, the baby may experience increased pressure on their head, compression of the umbilical cord, and other factors that can impede blood and oxygen supply to the brain.
As a result, brain cells may be damaged or die, leading to long-term consequences such as developmental delays, cognitive impairments, motor disabilities and cerebral palsy.
Timely intervention and proper monitoring during labor can help prevent or minimize the risk of brain damage due to prolonged labor.
Is there any treatment for newborn brain damage?
Treatments for newborn brain damage immediately after birth are aimed at preventing complications and developmental delays, and they may include the following options:
- Surgery. Surgery for newborn brain damage is typically only considered in cases where there is a specific structural abnormality or condition that can be addressed surgically, such as intracranial hemorrhage or hydrocephalus. The decision to proceed with surgery depends on the underlying cause of the brain damage and the potential benefits versus risks of the procedure.
- Hypothermic therapy. Also known as therapeutic hypothermia or cooling therapy, hypothermic therapy is a medical treatment used to help newborns who have experienced brain damage, particularly due to HIE. Hypothermic therapy involves cooling the baby’s body temperature to around 91 to 93°F for a specific duration, usually 72 hours after the baby’s birth. The cooling therapy works by reducing metabolic activity in the brain, which can help protect brain cells from further damage and reduce inflammation.
How cooling therapy impacts brain damage in infants
Cooling therapy is an essential treatment to prevent brain damage in babies who experience HIE caused by a lack of oxygen and blood flow to the brain during or shortly after birth. To be effective, cooling therapy should ideally be initiated within 6 hours of birth.
However, not all babies born with HIE should be given cooling therapy, including those who:
- Are born earlier than 34 weeks gestation
- Weigh less than 3.8 pounds
- Have an intracranial hemorrhage, blood clotting disorder, or septicemia
- Have certain genetic or congenital abnormalities
If your baby suffered brain damage after receiving cooling therapy and any of these factors apply, their injury could be the result of medical negligence.
What treatments are available to older children diagnosed with brain damage?
Toddlers and older children with permanent brain damage have many treatment options available that can help improve their overall health and quality of life, including:
- Medications for children suffering from conditions like seizures or attention-deficit/hyperactivity disorder (ADHD)
- Physical and occupational therapy to improve strength, coordination, and movement and help them function more independently
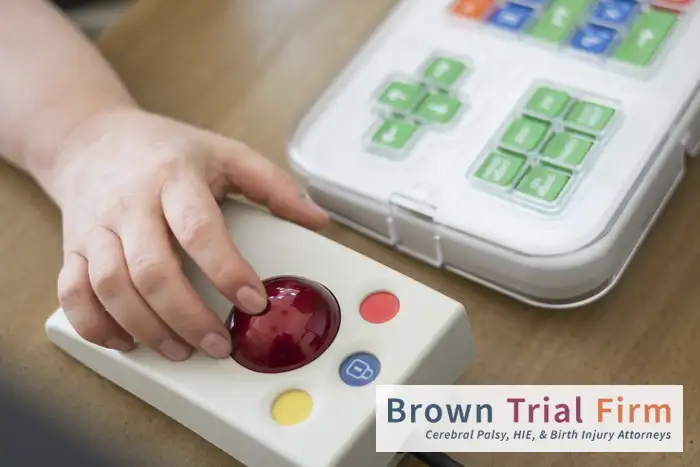
- Adaptive equipment like crutches, speech-generating devices, communication boards, and even adaptive clothing with unique closures, zippers or Velcro to aid in dressing
Best adaptive equipment & technology for kids with cerebral palsy
Learn about the newest innovations in adaptive toys, equipment and technology to help kids with cerebral palsy and other birth injuries.
Can a baby swing cause brain damage?
Baby swings aren’t designed to go fast enough to cause brain damage, especially when an infant is positioned correctly in the seat and buckled in. The real risk with baby swings occurs if you push them too fast (using a non-motorized version) or forget to fasten them in, which could lead to a fall.
Only using swings approved for infants and taking a gentle approach with little ones at the park is the best way to reduce the risk of a fall-related brain injury.
Can babies get brain damage from hitting their heads?
Yes, babies can sustain brain damage from hitting their heads, especially if the impact is significant or if there’s a forceful shaking motion involved.
Fortunately, babies are remarkably resilient, so the risk of brain damage from a mild isolated blow is fairly low. But it’s always best to have your baby evaluated by a doctor if you’re concerned about a fall or other injury involving their head.
What are the signs of brain damage in babies after a fall?
Your infant should always be evaluated for brain damage if they lose consciousness after a fall. You should also be concerned if they experience unusual sleepiness, vomit after the incident, or display signs of neurological symptoms, such as dizziness or altered vision.
Keep in mind that since an infant can’t tell you their head hurts, you’ll want to keep an eye out for prolonged crying that doesn’t stop with your usual calming strategies.
Could dropping a baby cause brain damage?
Dropping a baby could result in brain damage, depending on the circumstances. You’ll definitely want to take your baby to the emergency room if you dropped them from higher than 2 feet. It’s also crucial to check for brain damage if your baby landed on a hard surface, such as a tile floor or concrete. Looking for bumps on your baby’s head or changes in their behavior can help you recognize the signs of serious brain injuries.
Can leaving a baby to cry damage their brain development?
According to a recent report, studies haven’t been able to definitively prove a link between crying and long-term brain damage.
Although you generally want to tend to your baby when they cry to help them develop a sense of security and trust, you also don’t need to feel guilty if you can’t get to them right away or when you’re practicing a gentle form of sleep training.
How can the timing of a brain injury influence a baby’s development?
One recent study that tracked the development of 2 different groups of infants found that those who developed brain injuries in utero from prolonged oxygen deprivation caused by heart failure had worse long-term outcomes than those who had a lack of oxygen during delivery associated with HIE.
These results seem to indicate that shorter periods of oxygen deprivation lead to better prognoses for babies. While more work is being done to understand how trauma impacts long-term brain development, it’s clear that early intervention could help infants achieve better outcomes as they grow.
Can throwing a baby in the air cause brain damage?
Yes, throwing a baby in the air exposes them to a higher risk of brain damage for several reasons.
During the toss, it’s possible to miss catching your infant, which could lead to a blow to the head or a fall-related injury. There’s also the possibility that your baby’s head might move uncontrollably due to naturally weak neck muscles. In this case, they could develop brain injuries from the same back-and-forth motion that causes whiplash.
Concerned your baby’s brain damage was caused by medical negligence? Consult with our birth injury attorney.
Facing a brain damage diagnosis for your baby can be frightening. It’s common to feel overwhelmed as you try to figure out how to best support and care for your child and provide them with the essential treatment they need. As you work with your infant’s medical team, consider reaching out to an infant brain damage attorney who can help you manage the financial and legal aspects of planning for your child’s future.
As an experienced birth injury attorney, Laura Brown is deeply committed to advocating for families whose lives have been forever changed by preventable brain injuries during pregnancy and childbirth. That’s why she offers free consultations to answer your question and provide you with the legal guidance you need to make an informed decision about the next right steps in the process for you and your child.
Contact Brown Trial Firm today to find out if a birth injury lawsuit might be able to help your family get the much-needed compensation your child deserves.
References
Doucleff, M. (2019, July 15). Sleep Training Truths: What Science Can (And Can’t) Tell Us About Crying It Out. NPR.org. https://www.npr.org/sections/health-shots/2019/07/15/730339536/sleep-training-truths-what-science-can-and-cant-tell-us-about-crying-it-out
Neonatal Hypoxic-Ischemic Encephalopathy. (n.d.). Www.nationwidechildrens.org. Retrieved July 25, 2023, from https://www.nationwidechildrens.org/conditions/health-library/neonatal-hypoxic-ischemic-encephalopathy#:~:text=In%20severe%20cases%2C%20a%20baby
Ramirez, A., Peyvandi, S., Cox, S., Gano, D., Xu, D., Tymofiyeva, O., & McQuillen, P. S. (2022). Neonatal brain injury influences structural connectivity and childhood functional outcomes. PLOS ONE, 17(1), e0262310. https://doi.org/10.1371/journal.pone.0262310