Why you should consult with a birth injury attorney if your baby had a stroke during childbirth
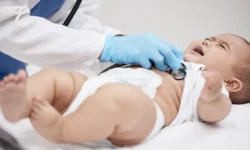
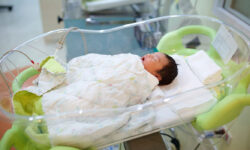
A neonatal stroke is a condition that interrupts the blood supply in a baby’s developing brain within the first 28 days after birth. While similar to strokes that adults experience, neonatal strokes are more difficult to detect since the baby cannot verbally communicate what symptoms they are experiencing, meaning doctors and parents have to be vigilant to identify these signs.
Seizures are the common symptoms of a neonatal or infant stroke. At times, a seizure can occur the first day after a child has been born. Other signs and symptoms of a neonatal stroke include:
- Hemiparesis – weakness on one side of the body
- Hypotonia – lethargy and extreme sleepiness
- Apnea – the child may stop breathing temporarily
- Difficulty feeding
- Neurological impairment
When a baby suffers from a stroke before or shortly after birth, they may not show any symptoms until much later on. They might experience balance difficulties or speech delays, which are signs that the child suffered from a stroke around childbirth.
If your child has a neonatal stroke, you should ensure they get the help they need within the shortest time possible. If treated early enough, the child may not suffer long-term health complications. If you suspect that your child suffered from a stroke, you should get in touch with a doctor, and they’ll guide you on how to go about the issue.
After they’ve been treated, consider consulting with a birth injury lawyer to find out if medical negligence played a role in your child’s stroke.
Common types and causes of neonatal stroke
There are a couple of different types of neonatal strokes.
The most common one is arterial ischemic stroke. This condition usually occurs when there is a structural abnormality or a blood clot. Structural abnormalities can include Moyamoya disease or other types of cerebral arteriopathies, causing the blood flow to be obstructed within the baby’s spinal cord or brain.
When bleeding occurs in the brain (medically known as a neonatal intracranial hemorrhage), the baby can experience a hemorrhagic stroke. Some possible causes of a hemorrhagic stroke include the presence of abnormalities in the blood vessels such as arteriovenous malformations, cavernous malformations, aneurysms and venous angioma. Certain clotting disorders, including sickle cell disease, hemophilia, congenital heart disease and brain tumors, can also lead to bleeding and result in a hemorrhagic stroke.
A perinatal stroke can occur to a baby starting at 20 weeks gestation and up to 28 days after birth, but these strokes are particularly common during the first week of life. Some estimates put the rate of perinatal stroke at about 1 in 2,200 live births. Perinatal strokes are caused by some oxygen-depriving event, and hypoxic-ischemic encephalopathy (HIE) commonly occurs at the same time.
How is a neonatal stroke diagnosed and treated?
There are cases where a neonatal stroke can be detected while the baby is not yet born. In such cases, there is a greater likelihood that a birth defect is the cause. The mother may have to undergo a fetal MRI to determine whether or not their baby has had a stroke in the womb.
If the stroke is severe, it should be detected through an ultrasound. After the child is born, further imaging should be carried out to confirm whether the child suffered a neonatal stroke or not.
If a newborn has a seizure, their head should be examined through a CT scan or an ultrasound. An MRI should be conducted as well.
The type of intervention and diagnostic testing will depend on the cognitive function impacted by the condition.
When it comes to immediate treatment of the condition, a neonatal stroke can be treated in several ways:
Therapeutic hypothermia
Therapeutic hypothermia is usually administered to a baby’s head. Commonly referred to as “brain cooling,” therapeutic hypothermia is when the temperature of the brain is lowered in order to purposely reduce brain activity. As a result, further damage to the brain is halted. The main advantage of this treatment option is that the brain won’t overheat because of increased blood flow.
Hyperbaric oxygen therapy
Hyperbaric oxygen therapy is a treatment where the infant is placed in a pressurized room full of oxygen. The pressurization enables the infant’s body to absorb more oxygen faster to make up for asphyxiation.
Both therapeutic hypothermia and hyperbaric oxygen therapy are effective but relatively new, so some medical practitioners shy away from them. The conventional treatment methods currently are heparin and urokinase.
Drugs: urokinase and heparin
Urokinase (also known as urokinase-type plasminogen activator) is a protein that usually comes from the human kidney cells. It’s also a clot-busting drug that is administered through an injection to help to dissolve unwanted blood clots.
Heparin is an anticoagulant (blood thinner) that also helps to reduce blood clotting.
Are neonatal and perinatal strokes preventable?
Most neonatal or newborn stroke cases occur within the first couple of weeks after a child is born or while they are still in the womb. To reduce the risk of your child suffering from a stroke in the womb, you should safeguard your health by eating healthy, staying hydrated and refraining from smoking. However, sometimes a neonatal stroke is not based on lifestyle factors, but congenital and genetic deformities.
For example, suppose there is a history of clot-related disorders in your family. In that case, your doctor may suggest you undergo some tests to determine whether you have a genetic disorder referred to as Factor V Leiden. This genetic disorder is specifically known to cause clotting in the fetus. Early detection matters for those with the genetic disorder, and medical professionals should take the necessary steps to manage the condition.
If your child (born or unborn) shows signs of a stroke, then a blood transfusion can be performed using blood that has been diluted in saline to prevent a neonatal stroke. This blood transfusion will help if the child has a high number of red blood cells because of childbirth complications or pregnancy.
When to consult with a birth injury attorney
The injuries, disabilities and conditions vary significantly when it comes to neonatal strokes. Some of the long-term effects can include seizures, cerebral palsy, epilepsy, developmental delays and motor function disorders.
If your baby has suffered from a neonatal stroke, you should get in touch with a birth injury lawyer as soon as possible. We will work closely with you and use our expertise in such cases to secure the compensation you deserve.
- Cerebral Palsy
- Caput Succedaneum and Cephalohematoma
- Neonatal Intracranial Hemorrhage (Childbirth Brain Bleeds)
- Hydrocephalus (Extra Fluid in the Brain Cavity)
- Cervical Dystonia
- Hemiplegia (Brain or Spinal Cord Injury)
- Hemorrhagic Stroke
- Neonatal Stroke
- HIE
- Periventricular Leukomalacia (PVL) Brain Injury
- Infant Seizures
- Spastic Diplegia (Spasticity in the Legs)
- Top Risks for Birth Injuries
- Fetal Alcohol Syndrome
- Facial Paralysis
- Spinal Cord Injuries
- Bell’s Palsy
- Brachial Plexus Nerves & Erb’s Palsy
- Klumpke’s Palsy
- G-Tubes for Newborns
- Medical Errors
- Cesarean Section & Birth Injury
- Negligence in Brain Cooling Treatment
- Craniosacral Therapy
- Occupational Therapy
- Speech Therapy
- Transition From Pediatric to Adult Healthcare
- Surgical Options for Spastic Cerebral Palsy
- Fetal Intolerance to Labor
- Jaundice (Kernicterus)
- Breech Position
- Placental Complications
- Umbilical Cord Problems
- Uterine Rupture
- Cervical Incompetence (Insufficiency)
- Blighted Ovum
- Necrotizing Enterocolitis (NEC) - Intestinal Inflammation
- Cephalopelvic Disproportion
- Meconium Aspiration Syndrome
- Amniotic Fluid Embolism
- Birth Injury from Premature Delivery
- Developmental Delays
- Abnormal Cord Insertion
- Infections at Birth
- Chorioamnionitis Bacterial Infection
- Premature birth
- Oxygen Deprivation
- Listeria
- Birth-Acquired Herpes
- Placenta Previa
- Placental Abruption
- Mismanaged Fetal Malposition
- Rapid Labor
- Obesity Related Birth Injuries
- Intrauterine Growth Restriction
- Blood Clots During Pregnancy
- Ectopic Pregnancy Misdiagnosis
- Myths & Facts About Birth Injuries
- Bacterial Vaginosis
- Gestational Diabetes
- Maternal Mortality Risk
- Oligohydramnios (Low Amniotic Fluid)
- Infections During Pregnancy
- Excessive Bleeding During Pregnancy
- Congenital Syphilis