Did your newborn suffer from brain damage due to a lack of oxygen at birth?
Talk to a birth injury attorney who has dedicated her entire career to these types of cases.
“They went above and beyond to give our family a level of closure that was vital for us to move forward...” - Della C.
“They worked their hearts out to get justice for a young child...I have been a lawyer for 20 years, and can honestly say that this law firm could be the best medical malpractice firm in the country.” - Reynaldo Garza III
lawyer
“I will definitely recommend them to any family. Laura is definitely hands down an amazing lawyer.” - Jacklyn C.
From the very first moment to our last, humans need to breathe. No matter what age you are, blood MUST circulate to deliver oxygen and nutrients to your cells and remove waste and toxic buildup. Without oxygen, your cells will die. If enough cells are affected, serious medical conditions, permanent brain damage or death can occur.
Although birth injuries happen in the earliest stages of life, they can result in damages that last for a lifetime. The expenses associated with long-term medical treatment for a birth injury are usually very extensive and can devastate the family’s finances.
If your child has sustained HIE or brain damage due to negligence, you may be entitled to compensation from the responsible party. However, you might understandably feel hesitant about pursuing litigation. Most hospitals and medical insurance companies are powerful entities with ample resources to employ highly-paid legal teams.
At Brown Trial Firm, we help even the playing field for patients by exclusively representing babies and their families. We’ll thoroughly investigate what happened. And if we believe the injury was avoidable and should have been prevented, then we will be ready to go up against even the largest hospital corporations or insurance companies. Years of devoted practice have instilled us with confidence, experience and the skills to match.
Have questions about a birth injury?
Verdicts & Settlements Financial security for Your Child
Birth injury cases are like babies—every one is unique and special. Although these past success stories are no guarantee of success in your case, they can provide you examples of what we’ve been able to accomplish in similar cases. Contact us to determine the value of your potential claim.
HIE Malpractice Lawsuit
The child’s HIE and CP were caused by hypoxia and ischemia when the umbilical cord wrapped around the child’s neck, preventing the child from getting enough oxygen. The medical providers did not identify the warning signs and did not order a timely c-section. The delay caused severe and permanent injuries.
Cerebral Palsy Malpractice Lawsuit
The child suffered HIE and CP injuries when the medical professionals failed to timely order and perform a c-section in response to fetal distress warnings. A contingent (%) fee charged on the successful recovery resulted in a fee of $3,080,000 and litigation expenses and attorney’s fees which were reimbursed by the client out of the gross settlement amount.
Cerebral Palsy Malpractice Lawsuit
The child suffered HIE and CP as a result of uterine rupture, placental abruption, and a delay in performing an emergency c-section. A contingent (%) fee charged on the successful recovery resulted in a fee of $1,441,584 and litigation expenses and attorney’s fees which were reimbursed by the client out of the gross settlement amount.
What is HIE?
Hypoxic-ischemic encephalopathy, or HIE, is a medical term for an injury caused by a lack of oxygen to a baby’s brain. “Hypoxia” means there isn’t enough oxygen in the blood. “Ischemia” means that not enough blood is flowing to the baby. “Encephalopathy” refers to the brain damage that is caused by the lack of oxygen flow to the brain.
HIE is a leading cause of cerebral palsy. HIE can also cause many other serious birth injuries, including autism, mental retardation and visual motor or visual perceptive dysfunction.
During pregnancy, labor and delivery, babies are especially vulnerable to lack of oxygen. During the vital perinatal period (the few weeks before, during and after birth), any interruption of oxygen to a baby’s developing brain is dangerous. Blood circulation is what supplies the body’s cells with oxygen for proper function.
There are 2 primary types of injuries caused by HIE:
- Hypoxia/ischemia. Oxygen deprivation causes cells to starve and die.
- Reperfusion injury. Oxygen deprived cells produce lactic acid and toxins. The lactic acid and toxins then re-circulate throughout the body via the bloodstream, causing additional harm.
Additionally, HIE can cause increased hyperactivity and attention disorders, and epilepsy. Other organs may be damaged, too, such as the heart, liver, kidneys and the central nervous system.
Severe cases of HIE may be identifiable immediately after delivery. However, sometimes HIE can go undetected until later, as the child grows older.
Before delivery
Out of the body’s entire oxygen supply, 20 percent is consumed by the brain. During pregnancy, the baby or “fetus” is not breathing with lungs. Instead, the mother’s placenta (an organ that develops and implants in the womb) and umbilical cord create a channel where blood circulates to and from the baby. Babies receive oxygen and nutrients, and also get rid of waste products and carbon dioxide, through the mother’s umbilical cord.
“Breathing” or gas exchange (i.e., oxygen for carbon dioxide) happens in the placenta itself in intervillous space. There, oxygenated blood from the mother diffuses into blood vessels in the placenta. The umbilical vein takes this blood to the baby.
The circulating blood bypasses the lungs and enters fetal circulation through special openings called “shunts.” The purpose of shunts is to bypass developing body parts (specifically, the lungs and liver).
The enriched blood comes through the umbilical cord and enters through a shunt near the baby’s liver called the “ductus venosus.” Some blood goes into the liver, but most travels on through the inferior vena cava into the right atrium of the heart. It’s then pumped out to the rest of the body in a “normal” circulatory pattern.
When the blood with waste products and carbon dioxide comes back to the heart, instead of being “oxygenated” by the baby’s own lungs, the waste is removed by 2 shunts—the foramen ovale (which bypasses the lungs) and the ductus arteriosus (which moves blood from the pulmonary vein to the aorta and on to the 2 umbilical arteries, back into the placenta for Mom to deal with).
During labor
During the birthing process, it’s especially important that the baby gets enough oxygen. Cells need oxygen to survive. If the baby doesn’t receive enough oxygen, the baby’s cells begin to die. If too many brain cells die, a brain injury occurs and the baby may have permanent brain damage.
Up until the umbilical cord is clamped at birth, the baby is still “breathing” through the mother’s umbilical cord. After the cord is cut, babies have to breathe on their own, with oxygen sucked in through the nose or mouth and pulled into the lungs.
With the first breaths of air, the baby’s lungs expand and the alveoli in the lungs are cleared of fluid. The resulting increase in the baby’s blood pressure and reduction in pulmonary pressure promotes the closure of the ductus arteriosus. That, in turn, increases pressure on the left atrium of the heart and decreases pressure in the right atrium, which stimulates the foramen ovale to close.
With these shunt closures, the baby’s circulation and blood flow through the heart just like everyone else. Sensors in the brain, carotid artery and aorta detect the carbon dioxide and oxygen levels in the newborn’s blood and send the data up to the brain stem, which regulates breathing. Other sensors in the airways, lungs and muscles also contribute to respiration.
When there are signs that the baby is not receiving enough oxygen, it may be necessary to deliver the baby quickly, either vaginally or by Cesarean section, to prevent injury to the baby.
After delivery
At birth, the doctor should carefully evaluate the baby’s condition and assign an Apgar score. The Apgar score is a subjective rating of the baby’s heart rate, skin color, reflexes, muscle tone and breathing effort. The doctor or nurse assigns a number from 0 to 2 for each item. The highest overall score is 10. A low Apgar score can indicate birth asphyxia.
An infant who has been deprived of blood flow and oxygen may have poor circulation, lethargy, abnormal breathing, blood-clotting abnormalities and lack of urine output. Physicians must act quickly to provide the proper treatment to help prevent further injury to the child.
What makes HIE so dangerous?
Sometimes the damage inflicted on a baby with HIE isn’t known quickly. This is because HIE can be difficult to diagnose when it occurs.
There are several reasons for this. A brain injury caused by HIE develops over a process. Blood pressure builds and oxygen is blocked from entering the brain. The brain cells begin to die and release toxic matter which will then damage other cells around them. HIE is dangerous because even if the cause of the injury is caught, this cycle of brain damage may continue for hours or even days.
Additionally, the extensive damage from HIE may not even be noticeable until developmental issues begin to occur later in the child’s life. There are many symptoms of HIE, but not all of them are extremely common or very apparent shortly after birth. A parent may notice that their child isn’t crawling or standing around the time they should be. Infants can be diagnosed with HIE as late as nine months after their birth.
Although tragic, the nature of HIE does provide some insight into how medical professionals must remain alert and follow the standard of care when delivering a baby.
When a baby suffers from brain damage, it is a traumatic experience for the entire family. Understanding the causes and signs is crucial for early detection and intervention.
In some cases, brain damage might be the result of medical negligence. This comprehensive guide will help you understand the various aspects of baby brain damage, from potential causes and symptoms to the legal options available if medical negligence is suspected.
What are the common causes of HIE?
Hypoxia or inadequate oxygen to the baby can result from a number of different known complications during pregnancy, labor and delivery.
For instance, during birth, HIE is possible through several different avenues: lack of oxygen, untreated jaundice, maternal infections, physical trauma and even low glucose levels. Lack of circulated oxygen can be the result of uterine contractions, compression or kinking of the umbilical cord, dangerous conditions such as uterine rupture or placental abruption, poor oxygen exchange or delivery from the mother to the baby through the placenta, as well as other conditions.
Here are some of the known causes of HIE:
Umbilical cord causes
The mother provides oxygen and nutrients to the baby in the blood that flows through the umbilical cord. If the umbilical cord is compressed or kinked, the flow of blood between the mother and the baby is either reduced or stopped entirely.
- Umbilical cord prolapse
- Nuchal cord (cord around the baby’s neck)
- Umbilical cord knot
- Umbilical cord abnormality
Placenta causes
The placenta is an organ of the mother’s body that is created during pregnancy. It exists inside the mother’s uterus. The placenta attaches to the inside of the uterine wall and attaches to the baby via the umbilical cord. The exchange of oxygen, carbon dioxide and nutrients between the mother and the baby happen in the placenta. There can be complications with the placenta that deprive the baby of adequate oxygen.
- Placental abruption
- Placenta previa
- Preeclampsia
- Uteroplacental insufficiency
Uterus causes
The uterus is the organ of the mother’s body that houses the baby during pregnancy. The uterus is a muscular organ that can contract and relax. There are different types of complications involving the uterus that can affect the flow of blood and oxygen to the baby.
- Uterine hyperstimulation or tachysystole
- Uterine rupture
- Uteroplacental insufficiency
- Vaginal birth after cesarean (VBAC)
- Cytotec or Misoprostol
- Pitocin
Other potential causes of HIE include:
Maternal causes
- Hypotension (low blood pressure)
- Hypertension (high blood pressure)
- Infections
- Infertility treatments
- Vascular or blood disorders
- Thyroid disorders
Fetal causes
- Fetal intolerance to labor
- Blocked airways
- Anemia
- Infection
- Cardiomyopathy
- Severe circulatory insufficiency
- Severe respiratory distress syndrome (RDS)
- Shock
- Fetal stroke
- Brain bleeds
- Macrosomia
- Cephalopelvic disproportion (CPD)
Delivery & labor room problems
- C-section errors or delays
- Physical trauma during labor and delivery including the use of forceps or a vacuum extractor
- Getting stuck in the birth canal
- Excessive pulling
- Breech extraction
- Dropped glucose levels
- Untreated jaundice
- Fetal monitoring errors or neglect
These are just a few examples of common complications that can occur during labor and delivery which cause hypoxia. Medical professionals must be well-trained to recognize these complications and to act quickly to protect the baby.
What are the symptoms of HIE during pregnancy?
One of the biggest symptoms of HIE during pregnancy involves fetal distress signals. These signals can usually be picked up by medical professionals during ultrasounds in virtually any trimester of pregnancy. A fetal distress signal is simply a movement or abnormal heart rate that a doctor can pick up on and treat accordingly.
Other signs and symptoms that doctors should take note of during pregnancy, especially a high-risk pregnancy, include:
- High blood pressure in the mother
- Unusual contraction patterns
- Little movement from the baby
- Extreme cramping in the mother, which usually targets the back
- Excessive vaginal bleeding
- Weight fluctuations that are extreme in the mother
The risk factors involved in a high-risk pregnancy vary. Some older women may be considered to have high-risk pregnancies. Women who have had previous birth complications or C-sections could also have high-risk pregnancies.
In the case of a high-risk pregnancy, a doctor will usually take special care to monitor both mother and baby throughout the entirety of the pregnancy.
It’s also worth noting that placental problems, such as placental abruption and placental insufficiency, can occur during pregnancy and during the birthing process. These conditions involve issues with the placenta dislodging from the uterine wall or a malformation of the placenta entirely. Again, in some cases, doctors may be able to pick up on this condition before it becomes a problem.
What are the symptoms of HIE immediately after birth?
Hypoxic-ischemic encephalopathy depends on 3 factors: the severity, timing and duration of the “insult” (cause of the injury). Some symptoms occur right away while others may not exhibit until later in life, making HIE difficult to diagnose.
Here are some signs that a baby is suffering from a neurological injury to the brain:
|
|
|
|
|
|
|
|
|
Mild hypoxic-ischemic encephalopathy may resolve. Moderate cases may or may not recover. Severe HIE cases often commonly result in:
- Stupor or coma (the infant may not respond to any physical stimulus except the most noxious)
- Irregular breathing and breathing support required
- Generalized hypotonia and depressed deep tendon reflexes
- Lack of neonatal reflexes (sucking, swallowing, grasping, Moro)
- Disturbances of eye motion
- Pupils that are dilated, fixed or poorly reactive to light
- Irregularities of heart rate and blood pressure, and death from cardiorespiratory failure
What are the symptoms of HIE during childhood?
Unfortunately, if an HIE diagnosis is not found within 24 hours of birth or suspicion of a brain injury is not followed up on, a child’s HIE may not be diagnosed until later in life. Because of the nature of HIE, major symptoms may not be very obvious immediately after birth.
Signs of HIE in infants and children include:
- Chronic seizures or epilepsy
- Seriously impaired motor skills
- Developmental delays and an inability to reach developmental goals
- Growth problems
- Impairments in hearing and seeing
- Trouble crawling, walking and moving in general
Cerebral palsy may be caused by HIE in some cases. Cerebral palsy can be diagnosed later on in development and treated accordingly.
How do I file a lawsuit for an HIE birth injury?
- Consultation. First, you should reach out to a birth injury attorney near you who is experienced in these types of cases to review the unique circumstances in your case and help determine if it’s worth pursuing. During this initial consultation, the lawyer will examine the circumstances surrounding your baby’s HIE injury and if medical negligence was to blame.
- Filing. If the attorney determines that you have grounds to file a claim, they can help you start the process by filing a lawsuit. At Brown Trial Firm, we typically begin this process by submitting a petition with the right court system.
- Discovery. During this pre-trial stage of the lawsuit process, our attorneys engage in “discovery,” which is when both sides in a claim exchange information about the case. This allows both sides to see what evidence the other side possesses, and can help to encourage a settlement negotiation before trial.
- Depositions. Another step we may wish to take before trial is conducting depositions, which is sworn testimony from a witness that might provide valuable information about your case. For HIE birth injury case, we commonly focus the deposition on what medical providers knew about the conditions which led to the brain injury before, during or after birth.
- Investigation. Throughout the lawsuit process, we will consult with experts in the medical field, such as respected physicians, maternity providers and nurses, to analyze the specific circumstances surrounding your case and establish if there was a failure in the standard of care which caused your baby’s HIE injury.
- Mediation. A majority of HIE injury cases avoid trial, and many are settled during mediation. During mediation, we will meet with the other party to try and reach a reasonable compromise or agreement out of court.
- Trial. Going to court should be a last-resort option because of the time and money required in going to trial. While we do everything possible to avoid trial, we’re also not afraid to take your case before a judge or jury if the defendant isn’t willing to settle or engage in mediation. Our experienced trial attorneys will present a strong case with the help of medical professionals and expert witnesses.
Filing a lawsuit is a serious action that you must carefully consider. During your free consultation, our HIE attorneys will help you weigh your legal options and determine if you have a strong case. Contact the Brown Trial Firm today to discuss your next steps.
HIE facts and statistics
- Approximately 20 per 1000 deliveries will require significant resuscitation, with biochemical and clinical evidence of perinatal asphyxia. Of these, only 1.6 per 1,000 will go on to develop signs of evolving encephalopathy consistent with hypoxic-ischaemic encephalopathy (HIE). This number is much higher in countries with limited resources.
- About 1-3 babies in 1,000 suffer an HIE injury at or near the time of birth. Approximately 15-20 percent of these babies with birth trauma will die after being born, and another 25 percent will have permanent injuries.
- Approximately 15-20 percent of infants are misclassified as having either a mild or no encephalopathy and are therefore not given treatment, which worsens their long-term prognosis.
- Birth asphyxia causes 23 percent of neonatal deaths worldwide.
- HIE is the fifth leading cause of death worldwide in children under 5 years of age, according to the World Health Organization.
- Among infants with moderate HIE, 10-20 percent develop minor neurological conditions, and 30-50 percent develop more serious complications.
- For infants with severe HIE, there is a 25-50 percent mortality rate. Deaths most often occur in the first few days after birth. Of babies that survive, roughly 80 percent develop serious complications.
- Approximately 30 percent of children with moderate-severe HIE develop cerebral palsy.
- Approximately 16 percent of children with moderate-severe HIE develop epilepsy.
- Approximately 14-17 percent of children with moderate-severe HIE experience blindness and 6 percent have hearing impairments.
- Hypothermia therapy should be started as soon as possible after the hypoxic-ischemic injury; current guidelines recommend that it begins within 6 hours of birth.
Sources:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4737695/
https://www.medscape.com/answers/973501-106461/what-is-the-global-prevalence-of-hypoxic-ischemic-encephalopathy-hie
https://emedicine.medscape.com/article/973501-overview#a2
Medical Mistakes Can Cause HIE. Is HIE preventable?
Yes, some cases of HIE can be prevented. HIE can be caused by a lack of oxygen, untreated jaundice, infection, physical trauma or low glucose levels, as well as by contractions, problems with the umbilical cord, uterine rupture or placental abruption and other conditions.
The medical term for when a baby doesn’t get enough oxygen is “asphyxia.” There are 2 types of asphyxia:
- Near-total or acute profound asphyxia happens when the baby is getting almost no blood flow or oxygen.
- Partial prolonged asphyxia occurs when a baby gets less oxygen than it needs for a longer period of time. Another term for this condition is “partial prolonged hypoxia.”
When a baby doesn’t get enough oxygen through acute or partial prolonged asphyxia and is asphyxiated, the baby can develop “metabolic acidosis.” Metabolic acidosis is a dangerous biochemical imbalance that occurs when the brain cells don’t have enough oxygen, which causes them to produce lactic acid through the process of anaerobic metabolism. Lactic acid damages the cells.
Many of the causes of HIE are entirely preventable with careful monitoring and quick treatment. It’s a sad reality that medical mistakes and doctor negligence are common causes of HIE.
Metabolic acidosis is detected by testing the baby’s blood. A sample is taken either from the umbilical cord or from the baby. The test then checks the pH and base of the baby’s blood for irregularities.
If your child was born with HIE, it may be due to a preventable medical error. Some errors that can result in HIE include:
- If your child was not timely delivered via C-section
- If your child was not given hypothermia treatment
If you have questions about your child’s HIE diagnosis, we may be able to help you find answers.
Hypothermia Therapy for Brain-Injured Babies
Even though neonatal cooling therapy is a widely proven and generally accepted treatment for newborns experiencing HIE, it’s important for medical providers to carefully follow strict procedures and steps to ensure the effectiveness of the therapy and avoid potential negative impacts.
Failure to follow these procedures can negate the treatment and cause further injury.
CAN THE BRAIN RECOVER FROM A HYPOXIC BRAIN INJURY?
The prognosis for patients who suffer a hypoxic brain injury can be difficult to predict. While some patients may seem to make a full recovery, the full effects of a brain injury are often not known until sufficient time has passed to observe the patient.
In cases with infants, it can be especially difficult to know the full effects of a brain injury because sometimes the effects are not known until years later. Parents may have to wait years to see whether their child achieves normal developmental milestones, then seek additional screenings and tests, all before having a full picture of the child’s health.
Furthermore, obtaining an appropriate treatment plan can help patients manage short- and long-term conditions caused by hypoxic brain injuries. In this sense, many patients can eventually recover from a hypoxic brain injury.
How is HIE diagnosed and treated?
Children with hypoxic-ischemic encephalopathy can experience serious brain damage and possible disabilities. The extent of brain damage depends on a number of factors, including:
- The severity of the oxygen deprivation
- The amount of time that the baby was deprived of oxygen
- The health and condition of the baby before the oxygen deprivation occurred
- How the baby’s health was managed after the oxygen deprivation occurred
HIE testing and diagnosis
Any signs of brain injury or abnormal neurologic function should be identified after birth. There are several tools used to diagnose this condition, including the APGAR score and the Sarnat staging score.
The APGAR score
APGAR stands for appearance, pulse, grimace, activity and respiration. This test is usually performed right after birth to evaluate the condition of the newborn.
The APGAR score takes into consideration paleness, heart rate, reflex responsiveness, overall muscle tone and breathing ability. Babies with HIE may exhibit pale or bluish skin, have a low heart rate and lack reflexes when tested. Some babies with HIE may also have little muscle tone and have problems breathing or crying after birth.
A very low APGAR score that does not improve in 5 minutes can lead to a diagnosis of HIE or possibly another birth injury condition. Unfortunately, given the subjectivity involved in the APGAR scoring system, HIE may not always be detected through this test.
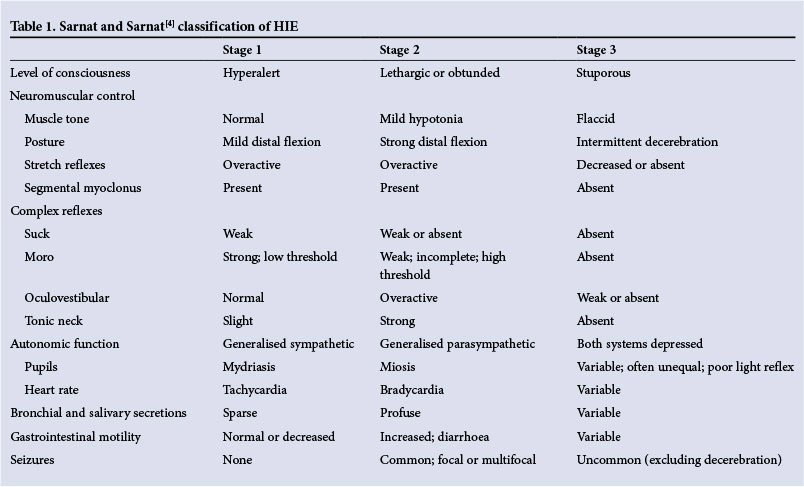
The Sarnat clinical stages of HIE score
In 1976, Sarnat and Sarnat were working on developing a clinical ranking system to help improve the diagnosis of hypoxic-ischemic encephalopathy. These doctors proposed a 3-stage system for classifying HIE.
Stage I
In Stage I, or mild cases of HIE, the infant’s symptoms right after birth include:
- Hyperalertness from the infant
- Slightly decreased muscle tone (floppy muscles)
- Brisk deep tendon reflexes (e.g. a knee-jerk reaction doctors test for)
- Fussiness
- Difficulty feeding
- Trouble sleeping
- Frequent crying
Often, these symptoms will disappear within less than 24 hours from the child being born. However, all symptoms of HIE should be carefully monitored and treated appropriately.
Stage II
In Stage II, or moderate to severe HIE, the infant may show symptoms of:
- Unusual lethargy
- Significant hypotonia
- Lower deep tendon reflexes (less reaction to reflex stimulus)
- Difficulty grasping with the hands
- Moro reflex (the feeling of suddenly falling, some people experience this right as they fall asleep—a baby will react to this sensation by shooting their arms out and may even gasp)
- Disinterest in sucking
- Trouble breathing or apnea (a momentary cessation of breathing)
- Seizures
In moderate to severe HIE, it’s very important that the child is properly monitored and treated. Effective medical care may significantly reduce the child’s prognosis. The first several weeks are the most critical period for monitoring and treating a child with Stage II HIE.
Stage III
In Stage III, or severe cases of HIE, the symptoms may include:
- An unresponsive, coma-like stupor
- No response to physical stimulus
- Extreme difficulty breathing
- Generalized hypotonia (floppy muscles over the whole body)
- Depressed deep tendon reflexes
- No neonatal reflexes (sucking, swallowing, grasping, Moro)
- Vision problems
- Dilated, fixed or unresponsive pupils
- Delayed seizures (increasing after 24-48 hours, resistant to treatment)
- Irregular heartbeat
- Poor blood pressure
Again, proper monitoring and treatment of Stage III cases of HIE are fundamental to improving the child’s condition. Severe cases of HIE may cause permanent injury or even death. It is the medical professionals’ duty to carefully watch the baby’s symptoms as they develop and to respond to symptoms of HIE with an effective treatment plan.
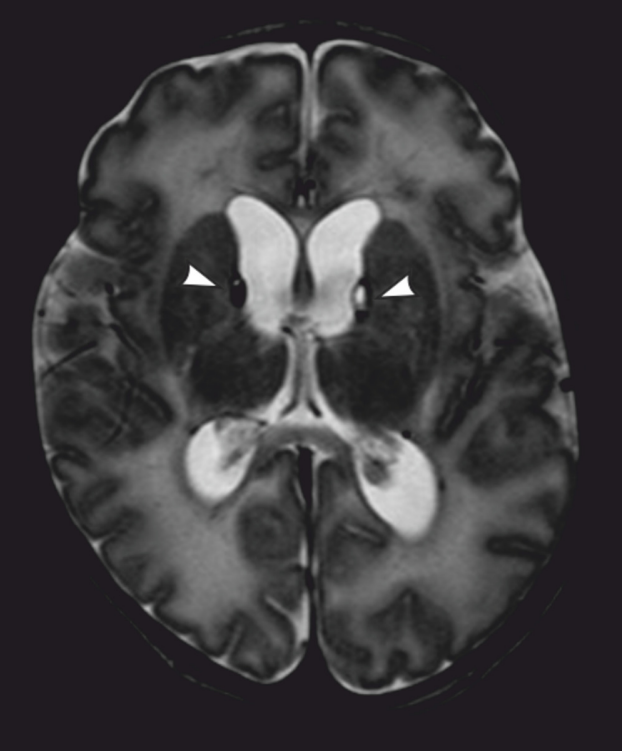
Laboratory tests, including those for arterial blood gas, coagulation system, cardiac and liver enzymes, renal (kidney) function and electrolyte levels, may be used to diagnose HIE. Neuroimaging through cranial ultrasonography (US), echocardiography and magnetic resonance imaging (MRI) is increasingly vital for early diagnosis. Of those 3, an MRI is probably considered the most valuable. Electroencephalograms (EEGs) may also be used to diagnose HIE since seizures are common. Hearing and eye exams may also be performed.
HIE treatment
Treatment for birth asphyxia depends on the severity. Babies born with mild asphyxia are provided with breathing support until they are breathing well on their own, and then monitored closely. Infants with more serious birth asphyxia may need a breathing machine, respiratory therapy and fluid and medications to prevent seizures and control blood pressure. Feedings may need to be delayed until the baby’s bowels recover.
Early intervention is vital.
Any type of fetal distress before, during or after birth should be handled swiftly by medical providers. When a baby isn’t getting enough oxygen, every minute matters. Doctors, nurses and midwives should know the signs that the baby isn’t getting enough oxygen and should be prepared to act quickly to protect the baby from injury and to prevent and mitigate brain injury and hypoxic-ischemic encephalopathy.
In cases of umbilical cord compression, prolapse or nuchal cord (when the cord is wrapped around the baby’s neck), the doctor may need to do a Cesarean section delivery to get the baby out quickly, getting him or her breathing as soon as possible. When the baby’s oxygen supply is diminished or cut off, it only takes minutes before long-term damage can occur.
Here are a few things that may help:
- Be aware of the risks associated with birth and delivery.
- Be observant during the birth process.
- Ask questions, and don’t be afraid to talk to the nurses and doctors about concerns.
- Insist on testing if anything seems off.
- If HIE is diagnosed, find out exactly what caused it.
Medical support provided to stabilize and treat HIE includes ventilation, perfusion blood pressure management (to prevent a “reperfusion injury” after the initial oxygen deprivation), fluid management, avoiding hypoglycemia and hyperglycemia, avoiding overheating, treating seizures and therapeutic hypothermia (~91°F for 72 hours).
Advanced treatment options for birth asphyxia include:
- High-frequency ventilation. This is a gentler form of mechanical ventilation that sends small puffs of air rapidly into the baby’s lungs. Unlike high-pressure conventional breathing machines, this type of breathing assistance is intended to protect a newborn’s fragile lungs from damage.
- Inhaled nitric oxide. This is used to treat respiratory failure and pulmonary hypertension (high blood pressure in the lungs). The nitric oxide goes directly into the windpipe through a breathing tube to help dilate blood vessels in the lungs so they can carry blood and oxygen to the body.
- Hypothermia. Cooling the infant’s internal body temperature to approximately 91 degrees Fahrenheit for up to 72 hours can help prevent brain damage during the second stage of asphyxia. This is the stage known as “reperfusion,” when normal blood flow and oxygen are restored to the brain. The treatment works best when started within 6 hours after birth. To qualify for hypothermia treatment, the infant must not be more than 4 weeks early.
- Extracorporeal membrane oxygenation (ECMO). A heart-lung pump may be used to provide temporary life support when the child’s heart and lungs are not functioning properly. The baby’s blood is drawn into a machine that adds oxygen, removes carbon dioxide and returns the oxygen-rich blood to the body. An infant on ECMO is sedated and closely monitored.
Glossary of common birth-related medical terms
- Anoxia: Complete lack of oxygen reaching the tissues (severe hypoxia).
- Asphyxia: Lack of total gas exchange (oxygen and carbon dioxide) causing suffocation.
- Encephalopathy: A disease, disorder or syndrome of overall effects on the function or structure of the brain.
- Hypercarbia (or hypercapnia): Elevated carbon dioxide levels in the blood.
- Hypothermia: Having a body temperature greatly below normal.
- Hypotonia: “Floppy baby syndrome” is a state of low muscle tone with very little flex or resistance in the muscles.
- Hypoxemia: Low oxygen in the blood.
- Hypoxia: Low oxygen in the tissues, representing a dangerous loss of oxygen to the brain or other body parts.
- Hypoxic-Ischemic (HI) brain injury: Injury due to hypoxia and/or ischemia (evidenced by biochemical, electrophysiological, neuroimaging or pathologic (postmortem) abnormalities).
- Hypoxic-Ischemic Encephalopathy (HIE): Encephalopathy with proof of damage specifically from a hypoxic and/or ischemic causes.
- Ischemia: Diminished/blocked blood flow to a part of the body.
- Neonatal encephalopathy: Clinical term that describes an irreversible injury-induced abnormal neurobehavioral state (decreased level of consciousness, signs of brain stem and/or motor dysfunction).
- Perinatal asphyxia: Condition during labor in which impaired gas exchange leads to fetal hypoxemia and hypercarbia.
- Perinatal/Neonatal depression: Condition of an infant within 1 hour of birth which includes depressed mental status, muscle hypotonia and possible disturbances in spontaneous respiration and cardiovascular function.
- Reperfusion injury: When blood flow/oxygen is recirculated into damaged cells, which causes them to release toxins that harm the tissues.
- Sequela: A medical condition or disorder that comes as a result of a previous injury or illness. From the Latin word meaning “that which follows, consequence.”
Contact an experienced and passionate HIE and birth injury attorney
If your child was hurt by HIE, you probably have a lot of questions. We can help you find answers, and help you understand your legal rights if a medical professional made a medical error when treating you or your baby. But don’t wait to act since the statute of limitations may bar your ability to bring a case if you wait too long.
Proper HIE treatment can be very costly, and not all medical or rehabilitation costs may be covered by medical insurance. Children who have suffered severe, irreversible brain damage due to hypoxia may require round-the-clock treatment and care. Our birth injury attorneys can help determine whether you are legally entitled to recover damages for negligent medical care. This vital legal compensation can help pay for medical bills, rehabilitation, therapy, expenses, lost earnings and physical pain and suffering.
At the Brown Trial Firm, we will fight to protect your child’s rights and ensure that you are fairly and fully compensated for your losses. If you would like to know if your child’s HIE was preventable, contact us to schedule your free case evaluation.
- Cerebral Palsy
- Caput Succedaneum and Cephalohematoma
- Neonatal Intracranial Hemorrhage (Childbirth Brain Bleeds)
- Hydrocephalus (Extra Fluid in the Brain Cavity)
- Cervical Dystonia
- Hemiplegia (Brain or Spinal Cord Injury)
- Hemorrhagic Stroke
- Neonatal Stroke
- HIE
- Periventricular Leukomalacia (PVL) Brain Injury
- Infant Seizures
- Spastic Diplegia (Spasticity in the Legs)
- Top Risks for Birth Injuries
- Fetal Alcohol Syndrome
- Facial Paralysis
- Spinal Cord Injuries
- Bell’s Palsy
- Brachial Plexus Nerves & Erb’s Palsy
- Klumpke’s Palsy
- G-Tubes for Newborns
- Medical Errors
- Cesarean Section & Birth Injury
- Negligence in Brain Cooling Treatment
- Craniosacral Therapy
- Occupational Therapy
- Speech Therapy
- Transition From Pediatric to Adult Healthcare
- Surgical Options for Spastic Cerebral Palsy
- Fetal Intolerance to Labor
- Jaundice (Kernicterus)
- Breech Position
- Placental Complications
- Placental Problems
- Umbilical Cord Problems
- Uterine Rupture
- Cervical Incompetence (Insufficiency)
- Blighted Ovum
- Necrotizing Enterocolitis (NEC) - Intestinal Inflammation
- Cephalopelvic Disproportion
- Meconium Aspiration Syndrome
- Amniotic Fluid Embolism
- Birth Injury from Premature Delivery
- Developmental Delays
- Abnormal Cord Insertion
- Infections at Birth
- Chorioamnionitis Bacterial Infection
- Premature birth
- Oxygen Deprivation
- Listeria
- Birth-Acquired Herpes
- Placenta Previa
- Placental Abruption
- Mismanaged Fetal Malposition
- Rapid Labor
- Obesity Related Birth Injuries
- Intrauterine Growth Restriction
- Blood Clots During Pregnancy
- Ectopic Pregnancy Misdiagnosis
- Myths & Facts About Birth Injuries
- Bacterial Vaginosis
- Gestational Diabetes
- Maternal Mortality Risk
- Oligohydramnios (Low Amniotic Fluid)
- Infections During Pregnancy
- Excessive Bleeding During Pregnancy
- Congenital Syphilis